OUTCOME EVALUATION IN SHOULDER SURGERY USING BODY-FIXED SENSORS
- Contact person: Kamiar Aminian
- People involved: Brian Coley, Cyntia Duc
- Partners: CHUV – DAL
- Funding source:

Context
The shoulder complex is a joint that provides mobility and stability to the upper extremities of the human body. Various diseases may affect the motor functions of this joint, leading to difficulties in performing daily activities. In that case, functional evaluation enables the assessment of disorder effects and treatment outcomes. In clinical settings, this evaluation is mainly performed by questionnaires and clinical scales. Although fast and simple, these questionnaires and scales are prone to patient’s interpretation and currently no score is universally recognised as a gold standard. In research biomechanics, measurement with standard motion capture systems enables an accurate evaluation of the functional ability. However the use of such elaborate systems is often time-consuming, complex and expensive for clinical applications. Moreover, these systems are restricted to the laboratory environment, and consequently may not represent the patient’s actual motor function during activities of daily living. To this end, wearable measurement systems offer a promising alternative for the objective assessment of joint function in daily conditions. In this context, the goal of this project is to devise an easy-to-use system based on body-fixed sensors to measure, analyse and evaluate objectively the shoulder function in both laboratory settings and daily conditions.
Evaluation in clinical settings
A wearable inertial system composed of tri-axial accelerometers and gyroscopes (Physilog®), fixed to both humerus, was used to extract kinematic scores from seven activities of daily life involving shoulder movement. By performing measurement on healthy subjects and patients (pre- and post-operatively), it was demonstrated that two kinematic scores enable a relevant evaluation of the shoulder before and after surgery: the P-score based on the product of acceleration and angular velocity and the E-score on the arm elevation. Additionally, a smartphone application providing the kinematic scores was devised. The developed application offers an accessible and user-friendly tool for the objective evaluation of the shoulder during routine clinical practice.
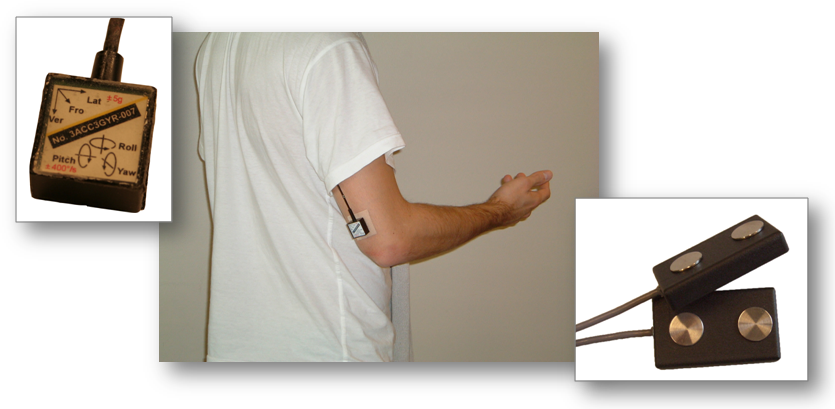
Figure: Measurement system on a participant: inertial modules (on the left picture) placed on humerus and surface electrodes (on the right picture) placed on trapezius superior, deltoid medial and biceps brachi.
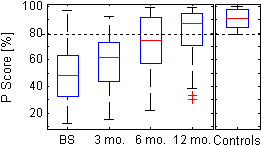
Figure: Boxplot of the P Score for the patients (41 patients, at baseline (BS) and at 3, 6 and 12 months after surgery) and for the controls (31 participants).
Evaluation of free-living activity
These inertial sensors, placed on both humerus and the trunk, were then used to monitor one day of usual activity. Several parameters were extracted and analysed from daily activity recorded from healthy subjects and patients (rotator cuff tear):
- The Working Level Score allows quantifying the ability to maintain the upper arm in elevated posture, based on the angle of elevation of humerus.
- The dominance focuses on the differentiation between the use of dominant and non-dominant arms.
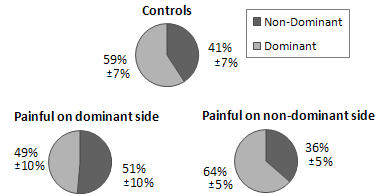
Figure: Use of the dominant and non-dominant sides, for the controls (41 participants), and the patients before surgery, divided in two groups: painful on the dominant side (12 patients) and painful on the non-dominant side (9 patients).
- The movements were analysed after a validation in a laboratory setting of a new method for detecting shoulder movements. The movement frequency and its symmetry index (ratio between both arms of one participant) highlighted a change of the index, followed by the recovery of the arm dominance after surgery.
- An approach based onthe cumulative distribution of the angular velocity of the arm movement illustrated an alteration in movement velocity due to the disorder.
Evaluation of the muscular activity
In order to assess the effect of a rotator cuff tear on the activity of the shoulder muscles, electromyography along with the movement measurement, using inertial sensors, were used simultaneously. The duration of muscular activation during movement was first evaluated in terms of reproducibility (test-retest) in a laboratory setting. Secondly, this duration revealed differences in muscular activation between pathological and healthy shoulders, during both imposed movements in the laboratory setting and during daily condition: for painful shoulders, the upper trapezius were activated longer, while the deltoid medial and biceps brachii were activated for shorter periods.
Conclusions
Based on a wearable measurement system, this work provides clinicians with new objective parameters that are relevant for the outcome evaluation of the shoulder function after surgery. On one hand, the parameters measured during specific activities in a clinical setting illustrate the alteration in the articulation mobility and function due to the disorder, and the recovery after treatment. On the other hand, monitoring in daily conditions quantifies the real use of the joint during free-living activities. These two types of assessment present complementary abilities and, together with clinical scores, contribute to an improved understanding and management of disorders and treatments for the shoulder joint.
Main publications
Coley B, Jolles BM, Farron A, Bourgeois A, Nussbaumer F, Pichonnaz C, et al. Outcome evaluation in shoulder surgery using 3D kinematics sensors. Gait Posture. 2007; 25 (4): 523-32.
Coley B, Jolles BM, Farron A, Aminian K. Arm position during daily activity. Gait Posture. 2008; 28 (4): 581-7.
Coley B, Jolles BM, Farron A, Pichonnaz C, Bassin JP, Aminian K. Estimating dominant upper-limb segments during daily activity. Gait Posture. 2008; 27 (3): 368-75.
Coley B, Jolles BM, Farron A, Aminian K. Detection of the movement of the humerus during daily activity. Med Biol Eng Comput. 2009; 47(5): 467-74.
Jolles BM, Duc C, Coley B, Aminian K, Pichonnaz C, Bassin JP, Farron A. Objective evaluation of shoulder function using body-fixed sensors: a new way to detect early treatment failures? J Shoulder Elbow Surg, 2011; 20(7): 1074-81.
Duc C, Farron A, Pichonnaz C, Jolles-Haeberli B, Bassin JP, Aminian K. Distribution of arm velocity and frequency of arm usage during daily activity: objective outcome evaluation after shoulder surgery. Gait Posture, 2013, in Press.