Multiple Sclerosis (MS) In-Patient Rehab Project
- Contact person: Gaëlle Prigent
- People involved: Prigent Gaëlle, Zhang Wei, Anisoara Ionescu
- Partners: Kliniken – Valens
- Funding source: Swiss MS Society

Background:
Gait disorders are common in patients with multiple sclerosis (PwMS). Multidisciplinary in-patient rehabilitation conducted by specialized doctors, nurses and therapists can improve the ability to walk by tackling the problem with various approaches: by increasing strength in leg muscles, by improving balance, by increasing cardio-pulmonary fitness, by fitting walking aids, by reducing fatigue and cognitive deficits, by working out strategies to compensate for impairments, and by optimising medical treatment. The scientific evidence for the effectiveness of in-patient rehabilitation is usually based on either clinical assessments of function (e.g. the 6 minute walking test) or on reports from PwMS, by using questionnaires (mobility or quality of life in daily life). Although clinical assessments provide important information about improvements of the functional capacity, they do not provide information about the impact of therapy on daily life
Aim:
We intend to observe the impact of in-patient rehabilitation on walking in daily life using miniature, wearable sensors, fixed on the shoes. Previously validated algorithms (Moufawad el Achkar et al, 2017) are used to extract Physical Activity (PA) metrics and gait parameters to quantify and characterize daily life behaviors and intense rehabilitation training effects.

Methods:
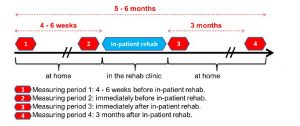
The physical and locomotor activity before and after in-patient rehabilitation will be measured in a longitudinal, observational study at 4 time points. At each time point, the physical and locomotor activity is measured during daytime over 7 successive days, during which the patient wears the sensors in daily life. The first two measuring periods (4 – 6 weeks, and immediately before in-patient rehabilitation) define the baseline locomotor behavior. The third and fourth measuring periods (immediately, and three months after in-patient rehabilitation) document the therapy impact on daily life, and the potential persistence of the therapy effect over three months.
Patients are asked to wear two inertial sensors (Physilog 5, Gait Up, CH) fixed on the shoes thanks to rubber clip. Classification algorithms that have previously been developed will be used to classify the type of activity (e.g. sitting/standing, walking, lying, stairs ascent/descent) [1] [2]. The algorithm was applied for the evaluation of rehabilitation programs in frail older adults suffering from hip fracture, as well as stroke patients [3]. This study will provide an interesting and rich dataset on MS patients, allowing us performing a clinical validation on this specific population.
Outcomes:
This study allows quantifying the impact of in-patient rehab on physical activity and walking in daily life in several dimensions: it will document the impact on the overall activity level, on walking episodes and on spatiotemporal characteristics of gait. We also aim at examining the relation between clinically assessed gait function as assessed by standard tests (e.g. walking speed in the 6min walking test) and daily life walking activity.
Main Publications:
- Moufawad el Achkar, C., et al., Instrumented shoes for activity classification in the elderly. Gait Posture, 2016. 44: p. 12-7.
- Moufawad el Achkar, C., et al., Physical Behavior in Older Persons during Daily Life: Insights from Instrumented Shoes. Sensors (Basel), 2016. 16(8).
- Achkar, C.M.E., Instrumented shoes for daily activity monitoring in healthy and at risk populations. EPFL Thesis, n° 7149, Chapter 6 and Chapter 7, 2016.